CARE & TREATMENT IN NEW YORK AND NEW JERSEY
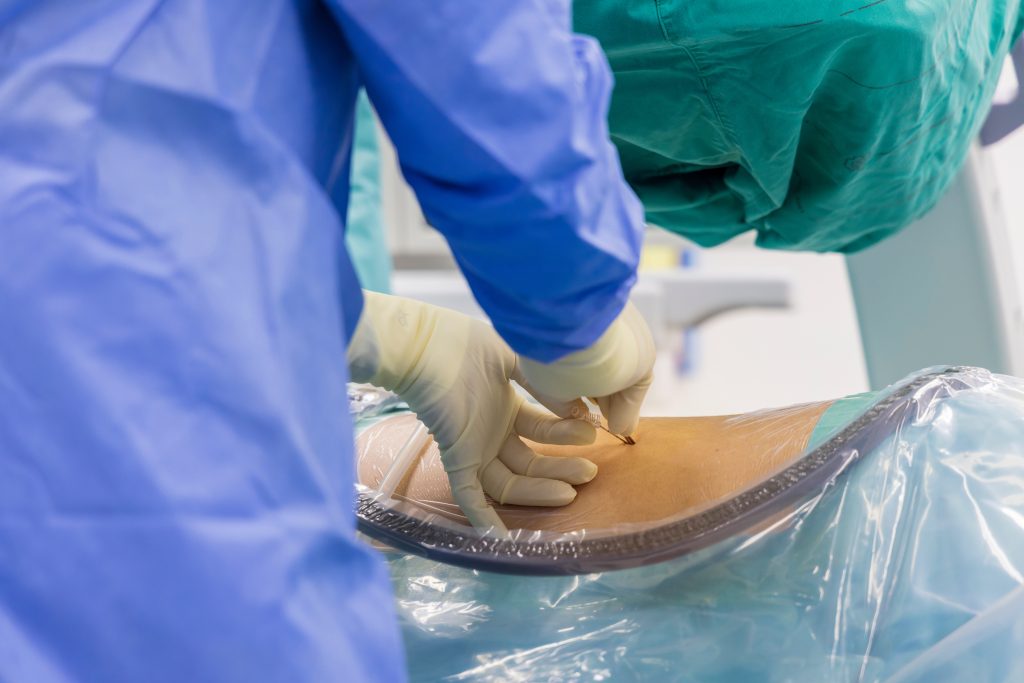
Chronic lower back pain radiating down your legs can make even the smallest movements, like bending to tie your shoes or walking up stairs, unexpectedly painful. When conservative measures like physical therapy and medication provide inadequate relief, lumbar epidural steroid injections offer a targeted intervention that delivers powerful anti-inflammatory medication directly to the source of nerve irritation, potentially providing months of significant pain reduction without the risks and recovery time of surgery.
At New York Spine Specialist in New Jersey, our physicians perform advanced lumbar epidural steroid injections for patients. Our comprehensive approach includes precise image guidance to ensure accurate medication delivery to the specific areas causing your symptoms. With convenient New Jersey locations, we provide accessible, specialized care designed to help patients experiencing lumbar radiculopathy, spinal stenosis, and other nerve-related back conditions achieve meaningful pain relief and improved function.
Lumbar epidural steroid injections (LESIs) represent a targeted interventional pain management approach that addresses nerve inflammation in the lower spine:
This minimally invasive technique delivers medication precisely where it’s needed most:
Unlike oral medications that affect your entire system, epidural injections concentrate medication directly around inflamed nerve tissue.
The therapeutic effects work through several complementary mechanisms:
While not a permanent solution for structural problems, these injections can provide significant symptom relief lasting from weeks to months.
Several specific spine conditions respond particularly well to this interventional approach:
When nerve roots become compressed or irritated in the lower spine:
Epidural injections can significantly reduce this nerve inflammation, often providing substantial relief from radiating symptoms.
This condition involves the narrowing of the spinal canal that houses nerve structures. Progressive narrowing places pressure on the spinal cord and nerve roots. Patients typically experience pain or cramping in the legs when walking or standing. Symptoms often improve with sitting or leaning forward. Epidural injections can reduce inflammatory swelling in the narrowed areas, potentially improving walking tolerance and standing comfort.
When disc material protrudes and contacts nearby nerves:
Injections can address both the chemical irritation and inflammatory response, potentially providing significant relief even if the structural herniation remains.
As intervertebral discs deteriorate over time:
Epidural injections can calm this inflammation, potentially interrupting the pain cycle, while other treatments address the underlying degeneration.
This interventional approach offers several distinct advantages for patients with appropriate conditions:
Epidural injections provide significant therapeutic benefit with minimal intervention:
This minimally invasive nature makes epidural injections an excellent option before considering more invasive surgical interventions.
Beyond therapeutic benefits, these injections provide valuable diagnostic information:
This diagnostic information proves invaluable in developing comprehensive treatment plans for complex spine conditions.
Epidural injections create therapeutic windows for other treatments:
This synergistic effect with rehabilitation often produces better long-term outcomes than either approach alone.
Our New Jersey specialists employ contemporary approaches that enhance traditional epidural injection techniques:
Several specific approaches allow for targeted medication placement:
Our physicians select the optimal approach based on your specific pathology and symptom pattern.
Advanced visualization ensures accurate medication delivery:
These imaging technologies substantially enhance both the safety and efficacy of the procedure.
Patients choosing lumbar epidural injections at our New Jersey locations can expect a streamlined experience:
Thorough preparation ensures optimal procedural outcomes:
This preparation helps ensure both safety and effectiveness.
On the day of your injection, established protocols ensure comfort and efficiency:
Most patients have minimal discomfort during this procedure due to local anesthesia and skilled technique.
Following your injection, structured protocols guide your immediate recovery:
This comprehensive approach optimizes both safety and therapeutic benefits.
Understanding the typical response pattern helps set appropriate expectations:
Individual responses vary based on your specific condition, inflammation severity, and other factors.
Patients commonly have several questions about this procedure:
Treatment protocols typically involve:
This individualized approach maximizes therapeutic benefits while minimizing unnecessary procedures.
All medical procedures carry some risks. The following are side effects you should know:
Our protocols minimize these risks through sterile technique, imaging guidance, and careful patient selection.
Most patients can resume light activities quickly:
Individual recommendations depend on your specific occupation and response to the procedure.
Lumbar epidural steroid injections offer a valuable treatment option for patients suffering from inflammation-related back and leg pain. At New York Spine Specialist, our board-certified physicians are rated in the top 1% of doctors in NY/NJ and are affiliated with prestigious institutions, including Hudson Regional Seacaucus, Carewell Health Medical Center, and other recognized hospitals throughout the region.
Our multilingual staff speaks Spanish, Italian, French, Korean, Cantonese, and Mandarin to ensure clear communication throughout your care. For a personalized evaluation of your spine condition and to determine if lumbar epidural injections might be appropriate for your situation, call our New Jersey office at (551) 550-7246 or connect through our contact form.